Imagine your baby has just been born.
Imagine that even though you want to hold your baby more than anything in the world, you are told you can’t.
Imagine that for the next couple of months you aren’t allowed to have your baby lie on your bare chest, letting that oh-so-soft skin touch yours as you form a life-long bond.
It’s something so horrible to imagine that a group of neonatal intensive care unit staff at Royal Columbian Hospital in New Westminster decided to imagine a solution.
The problem is when premature babies are using a high-frequency jet ventilator in order to breathe. That ventilator – which provides a jet stream of air through a baby’s lungs - is placed inside an incubator. It has a humming, thumping beat to it, meaning it disrupts the baby’s sleep because it normally has to be placed next to the patient’s head due to the limited length of the tubing.
Those limitations also mean preemies can’t be taken out of the incubator to be held while they’re on a ventilator.
It was this situation that led the NICU staff and RCH clinicians and respiratory therapists to sit down in 2016 and brainstorm a solution. Once they came up with a possible fix, they did what every great inventor does next.
They went to Canadian Tire.
Dallyce Varty, a clinical nurse educator at RCH, said they took “random pieces” from around the NICU, such as an IV pole, and bought bungee cords at Canadian Tire to strap down the part of the ventilator that normally goes inside the incubator.
Once the prototype was assembled, they tested it out.
“We were very encouraged with the results,” said Varty.
With a prototype in hand, the NICU staff applied for and received a $3,000 Fraser Health innovation grant in 2018 to build a more sophisticated model that includes a secure base and an arm that swivels as the baby is taken out of the incubator and placed in the loving arms of a parent.
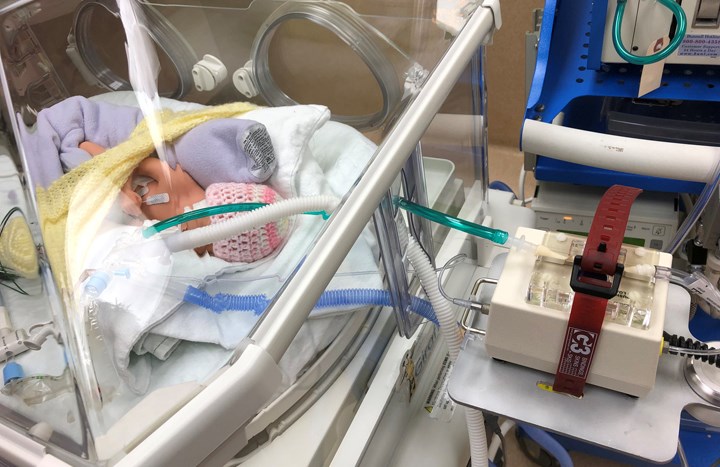
“If we hadn’t invented this, parents wouldn’t be able to hold their babies at such a crucial time,” said Varty.
Skin-to-skin contact has been shown to produce numerous benefits for both baby and parents. Aside from the bonding factor, this contact is a great stress reducer and facilitates the production of breastmilk – something that is difficult for a mother when their baby is born premature.
The device has been so successful, there are plans to produce three more at RCH. The intellectual property of the design is being transferred over to the RCH Foundation, which will be raising money for the three additional devices.
Varty and respiratory therapist supervisor Kuljit Minhas have also been busy travelling around the world to speak about the device.
Helping spread the word is Ashley Durance, a Chilliwack mother whose daughter Hazel was a patient at the RCH NICU after being born at 23 weeks and weighing under a pound.
Durance said Hazel was born so early, she hadn’t even felt her daughter kick inside, a situation followed by weeks of not being able to hold her baby.
“There was a definite disconnect there,” Durance said. “It’s so hard. This feeling of natural regret just comes over you.”
Then the first prototype was introduced and Durance was able to have Hazel lay on her bare skin at 32 days.
“It felt like she was back home where she belongs,” said Durance, who has blogged about her experiences and helps counsel other moms of premature babies. “That first moment, my husband says he’s never seen me smile that big. It still gives me goosebumps.”
Durance talks about skin-to-skin contact in this video:
Hazel is now an active toddler looking forward to her third birthday. Meanwhile, Durance has volunteered to be a spokes-parent for the RCH NICU device because she is so grateful for its invention.
“When I read another parent asking online about how to deal with the struggles of having a premature baby, I think, ‘This is why we’re doing this,’” said Durance. “It’s so important to spread the word to help others.”
Varty agrees. Her hope is that by speaking at conferences, other NICUs around the world will develop their own devices.



