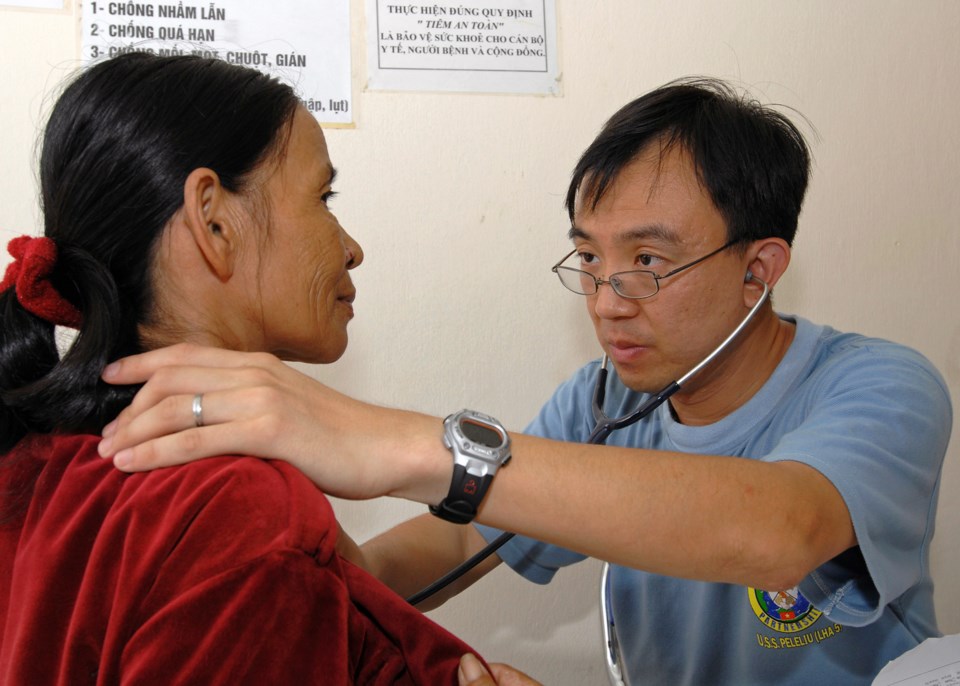
The Vancouver Native Health Society clinic is not accepting any new patients unless, that is, they are children, or have HIV/AIDS or have an emergency — as Jack did.
He’s a 79-year-old who recently moved here from Victoria. He suffered a stroke on the street, got shipped to St. Paul’s Hospital only to discharge himself. Monday — apparently with nowhere else to go — he turned up at the Downtown Eastside clinic at 449 East Hastings. And, of course, they took him in as a “one time visit” but you can bet he’ll be back.
And so will some 4,000 residents of the Downtown Eastside, 60 per cent of whom are First Nations. They view the clinic as their primary health care provider. And about half of them have been assigned a specific doctor who manages their file.
What Jack found and what I saw when I visited a few day later was a building that looked a bit rough on the outside, but inside is, as clinic administrator Tina Braun pointed out, it had “all the bells and whistles” you would find in most any doctor’s office anywhere in the city.
The clinic’s executive director Lou Demerais has been with this project from the beginning. He recalls the days when he was working for the Union of B.C. Chiefs and formed an organization in 1991 to inherit what was a small medical clinic on Main Street. It was only open evenings and was being run by a brash young social worker named John Turvey who gave Vancouver its first needle exchange to confront the spread of HIV/AIDS.
With Demerais and his society’s board, the clinic expanded its hours and moved to its present location. It includes a satellite clinic across the street that manages 575 HIV/AIDS patients.
Demerais considers its mission is to deal with all aspects of “wellness.” Braun says it is a “one-stop-shop” that includes everything from nutrition advice to housing assistance.
While they are splitting at the seams, the society’s ambition is to take care of anyone who walks through the door.
There are now a dozen doctors on salary rotating through three at a time and funded by Vancouver Coastal Health. (There are many more doctors who have offered their services but there is just no more room.)
There are elders available to smooth relations between patients and doctors. There are special clinic hours on Wednesday afternoons to serve women and children.
And not to be out done, the men created a Dude’s Club which meets with Dr. Paul Gross every other Thursday to deal with men’s issues — everything from prostate problems to relationship issues.
The clinic also has a mental health team and childcare specialists who are deployed to local community centres to run early childhood development programs.
There are also nurse practitioners, and aside from the space problem, more would be taken on but there is no sustainable funding available from the province to make that happen.
There’s a small well equipped kitchen that can feed 200 people a day. There is also an agricultural program out at the UBC farm (which has recently run out of funding) where First Nations folks are brought out from the Downtown Eastside, learn to grow their own food, smoke salmon and cook communal meals in the farm’s kitchen.
There was a diabetes program to deal with the many First Nations people who suffer from this disease in part as a result of poor diets. (Demerais says there are native communities in B.C. where 90 per cent of the population is diabetic.) That program, too, is no longer being funded by the federal government.
In the same way Jack found this place, people from all over the province — and beyond — but particularly in aboriginal communities know about Vancouver Native Health. There is, in fact, an informal network of these clinics in B.C.
But as successful as this clinic is, if it is to meet the needs of the community it serves, it requires more space and considerably more funding. This is particularly the case if it is to be part of achieving the province’s long-promised but now seemingly exaggerated goal of providing a family doctor for every British Columbian that needs one by 2015.
agarr@vancourier.com
twitter@allengarr