The number of people who died of a drug overdose in British Columbia in 2019 decreased by 36 per cent from the previous year but emergency calls for overdoses increased by two per cent.
Statistics released Monday by the B.C. Coroners Service at a news conference in Victoria revealed 981 people died of an overdose in the province last year, a decrease from 1,543 in 2018 and 1,495 in 2017.
In Vancouver, 245 people died last year.
At the same time, calls answered by paramedics to overdoses increased by two per cent in 2019 over the average of 24,000 per year, said Lance Stephenson, director of patient care delivery with B.C. Emergency Health Services.
“I can only speculate that we’re doing a better job at saving lives of the people that are overdosing,” said Stephenson, noting that prior to the widespread emergence of fentanyl in 2016, paramedics responded to 10,000 to 12,000 overdose calls per year in the province.
Stephenson said paramedics have been averaging 16 overdose calls per day in B.C. but that increases to 130 per day on welfare cheque day and the days that follow users collecting social assistance.
The conclusion from health experts for the decrease in deaths is that harm reduction measures such as the widespread use of the overdose-reversing drug naloxone, medication-assisted treatment and the opening of drug injection sites helped keep people alive.
In addition, B.C. Provincial Health Officer Dr. Bonnie Henry said some drug users have developed a tolerance to fentanyl, the synthetic opioid connected to 85 per cent of the 981 deaths in 2019 and 87 per cent of deaths in 2018.
“As fentanyl flooded the streets, and people were not used to it, we saw a lot of people die — even people who had long-term opioid addictions,” Henry told reporters.
“We do see people who are now dependent on fentanyl, and it’s even more challenging in some cases for people to recover from fentanyl addiction than from other opioid addictions. So the challenge has become worse in many ways.”
A statistic that wasn’t shared Monday and still being researched is how many overdose survivors now have a long-lasting brain injury or associated injury to almost dying.
The B.C. Centre for Disease Control will soon release data on this unknown statistic, according to Dr. Perry Kendall, who recently retired as provincial health officer, and attended Monday’s news conference.
“We’re only just beginning to really understand the full impact of this emergency and what the long-term effects will be on those who survived,” said Kendall, who is now co-interim executive director at the B.C. Centre on Substance Use.
“What we do know already is many hundreds of overdose survivors will need a lifetime of care and the resulting health-social-justice system supports that we will need will be a tremendous burden on all British Columbians.”
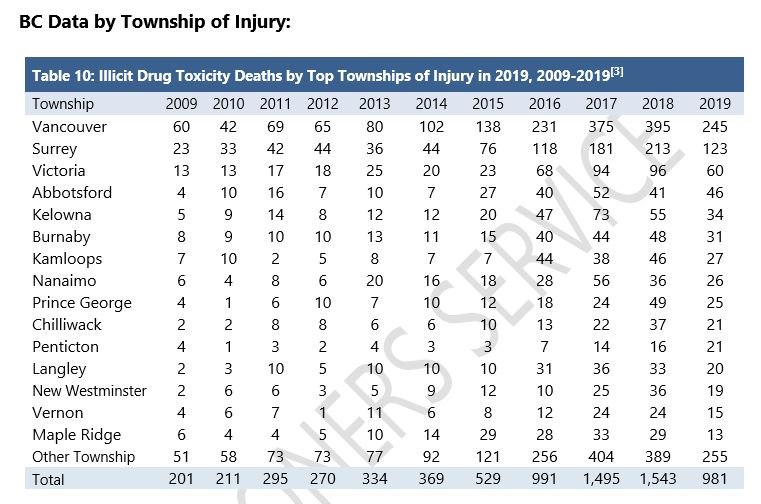
The 981 deaths recorded last year, which are expected to rise once further toxicology reports are completed, almost matches the 990 that occurred in the province in 2016 — the year the provincial government declared a public health emergency.
The 990 deaths recorded that year were a substantial increase from the 529 in 2015 and 369 in 2014. Overdoses killed 334 people in 2013 and 270 in 2012 in B.C.
It was on Thanksgiving Day in 2014 in Vancouver when the presence of fentanyl became a widespread concern to health experts. That’s when the opioid was detected in an unusually high number of overdoses at the Insite supervised injection site on East Hastings.
The Courier asked Kendall in a telephone interview after the news conference whether the reduction in overdose deaths last year is at all connected to the fact there are now fewer drug users in the province.
The question was based on the fact that more than 5,000 people died in B.C. of a drug overdose between 2016 and 2019, with Vancouver seeing the highest number of deaths.
The B.C. Centre for Disease Control, using data from 2015, estimated the number of injection drug users in Vancouver at 8,500 people. Province-wide estimates were not available at press time.
“That’s a good question, the answer is we don’t really know,” said Kendall, although he added that it is likely among the factors that explain a decrease in deaths, but not the major reason.
Judy Darcy, the Minister of Mental Health and Addictions, said the decrease in deaths is encouraging, but acknowledged the government has to continue with its initiatives to reduce the death toll.
“We still saw 981 people die last year — that’s two or three people every single day in British Columbia,” she told reporters in a news conference separate from the release of the overdose death statistics.
“We are not giving up, we are not slowing down. This is still a public health emergency and our overdose response as a government will continue firing on all cylinders.”
She said the combination of naloxone, injection sites and medication-assisted treatment — where 3,500 people have been prescribed opioid agonist treatment since July 2017 — are among the reasons that averted more than 5,000 deaths since the crisis began.
Darcy said calls to decriminalize drugs is a decision that can only be taken by the federal government. On the call for a “safe supply” of drugs, the minister said the B.C. government has significantly scaled up access to prescription alternatives to street drugs.
“We hope to be making an announcement soon with the federal government about increased access to other forms of safe prescription medications,” she said.
At Monday’s news conference, Chief Coroner Lisa Lapointe said 747 of the 981 who died last year were men, between 30 and 60 years old, and 234 were women.
They ranged in age from 13 to 76.
Lapointe shared brief stories of some of those who died, including a 42-year-old woman who was living with a mental illness and addiction.
“She was found deceased in the living room of her home by her child,” said Lapointe, noting toxicology tests confirmed fentanyl and amphetamines were detected in her blood.
“She is survived and grieved by her husband and two children.”
Added Lapointe: “Those who died of drug toxicity this year are more than statistics. They’re people, they were loved, they had hopes and dreams and challenges just like the rest of us.”
Meanwhile, the First Nations Health Authority is expected to release data in the coming weeks about the impact the overdose crisis is having on Indigenous peoples in B.C.
Data released in August 2017 showed Indigenous peoples are three times more likely to die from a drug overdose than a non-First Nations person and five times more likely to overdose.
@Howellings



