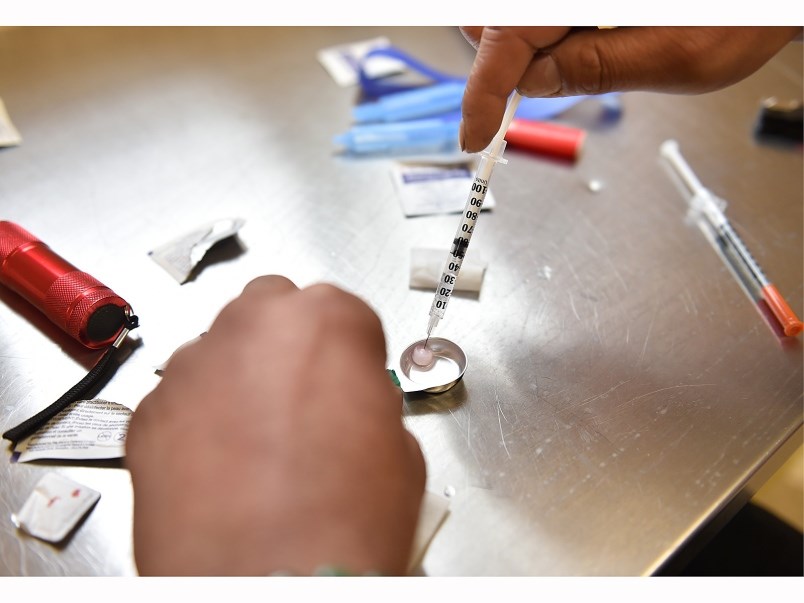
Re: “Doctors call for ‘heroin compassion clubs’ to reduce overdose deaths,” Feb. 28.
The B.C. overdose rate is unacceptable and requires drastic measures; heroin compassion clubs are not the solution. 2017 saw 1,487 people die, while 2018 saw 1,489. Continuously perpetuating this addiction cycle is absurd.
Compassion is great, but how is this venture compassionate? The compassionate approach is one where people who are stuck in the grips of addiction are offered a viable way out. Addicts are not suffering from a terminal illness, nor are they palliative care patients. These are humans stuck in a seemingly never-ending rut.
They can claim all day that the restrictions on who could buy would be strict, but how is that even enforceable? These clubs will lower barriers, but how will they distinguish between the experimenter and addict?
Very few people are against increasing quality of life through prescriptions. These clubs have nothing to do with prescriptions and would cost the user money, thereby overlooking associated societal issues.
Let’s start the reasons this won’t work with drug potency. Just hearing the word fentanyl makes the average person uncomfortable, but this substance is entrenched. Addicts seek the strongest possible high and fentanyl provides that, however unfortunate that may be. Overdose is the last thing on their mind.
The black market is a well-oiled machine. We don’t really believe people want to drive and line up when they can just call a dial-a-dope drug dealer, do we? The end users who are dying from these overdoses value time and their ability to be discreet. Unless this model undercuts in both price and convenience, it won’t catch on.
Do we want cocaine, crack, methamphetamine and fake pharmaceuticals to be available at these clubs? They all contain fentanyl and cause overdoses. For this model to work, it’s an all-or-nothing type of thing. I don’t think your average British Columbian has an appetite for something that drastic. The legitimacy that a project like this offers drugs is dangerous. Perception matters; heroin is bad and does ruin lives.
The societal impact of addiction is too often forgotten. It costs society money and the people suffer. Addicts are trapped in the cycle, struggling to support themselves and unable to see a way out. Instead of accepting widespread addiction and facilitating continued use, let’s offer a real solution.
British Columbia has fallen grossly short on providing inpatient rehab and evidence-based treatment. The success stories and long sobriety achieved are plentiful. When shown a way out, people often take advantage of it.
Access to treatment ought to be a fundamental right of every British Columbian.
Roughly $45,000 per year is what an addict costs society at present, how about us paying up front for rehab? The yearly expense could become a one-time cost. Addicts get their life back and society gets a taxpaying contributor.
The wait time for a government-funded bed is often multiple months long. Lower and middle-class families are asked to take on debt to pay. This is unacceptable and has to stop. Proven treatment ought to be available for people suffering from addiction, just like it is for people suffering from any other disease. The British Columbian life-expectancy has declined for the first time in many decades because of this crisis.
When people get into recovery they get their lives back and look forward to being honest, hardworking members of society. Families are reunited. It’s high time for us to pay for a solution that might actually have a lasting impact. Let’s take a progressive view — enough of being reactionary. This is a health crisis and the Ministry of Health needs to step up.
Stacy Wilson and Tristan Elliott,
Executive director and communications coordinator,
Together We Can Addiction Recovery and Education Society